Dental Issues after 50 - Things to Know
Improvements in dental health for patients 50 years and older
For Australians who have access to dental care and can afford regular dental examinations/treatments when required, it is likely that the current generation in the workforce will retain a large number of natural teeth as they turn 50 years and older in age. Unfortunately, this improvement in dental health is not seen uniformly across all groups of the population. We still see far worse dental health issues in indigenous Australians, specifically those from the Torres Straight Islands and in some immigrant communities. The contributing factors to this unsatisfactory situation are highly complex and involve many financial and political issues. The improvements seen in dental health in Australia and in developed countries worldwide is a result of a number of different factors. These include the availability of fluoride-containing toothpaste, fluoride mouthwashes, fluoridation of some water supplies, advances in dental materials technology, education on the dangers of frequently consuming sugars and fizzy drinks, with preventive dental health education largely provided in the dental practice.
Discoloured, stained teeth for patients 50 years and older
As we age, especially from age 50 years and beyond, our teeth often appear to become darker or even yellow in colour and consequently less attractive. Despite regular brushing, the teeth will not return to the white shade that you remember from earlier in life. Even using teeth whitening products from the chemist fail to make a noticeable difference. The answer is to see your dentists and discuss the various options that may help improve tooth colour. There are a number of options that can achieve the appearance and smile you want, some of which are relatively low cost. By the time your 50 years old, you may find the years of drinking coffee, tea, red wine, eating foods cooked with spices, and still sadly smoking, has caused tooth staining. The stain that attaches to the surface of teeth can be removed by the dental hygienist using innovative technologies such as the AirFlow device, which works toward removing stains on the exterior of the tooth in an efficient and comfortable manner. It is not only staining that discolours teeth. The consumption of acidic foods and beverages over many years can also result in the gradual dissolution of the white enamel that covers the teeth, consequently leading to the exposure of the underlying dentine to the oral cavity. Dentine makes up the majority of the tooth structure and is darker than enamel. It is also porous and rough, unlike the smooth enamel surface that once covered it. This dentine porosity and rough surface attract stain, plaque and calculus (tartar) far more quickly than the smooth enamel did in the past. The only way in which this can be managed is to clean the dentine, and then bond on a covering of a high impact composite tooth coloured filling material of a shade that matches the remainder of the tooth enamel.
Enamel damage and wear prevention
For individuals who suffer from acid reflux, frequently vomits (E.g. patients with anorexia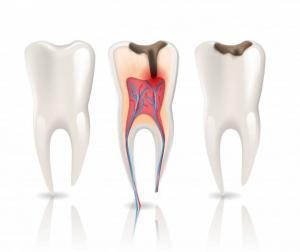 bulimia or in people who drink excess alcohol), or consumes large amounts of acidic foods or drinks, especially fizzy drinks, will suffer from significant damage to the enamel. This will leave the teeth with a worn appearance, poor in colour, often temperature sensitive with a gradual wearing away of the teeth simply from chewing or grinding teeth against one another. Plaque build-up occurs more quickly on dentine and stained tooth surfaces leading to an increased risk of new tooth decay and gum disease. This is a common finding in ageing adults but should not be considered a normal or acceptable change associated with ageing. These changes can be prevented if they are identified at an early stage. Such detection can only be achieved if adults attend for regular dental examination and dental health assessment. In other words, you don’t have to live with a yellow, dull smile!
bulimia or in people who drink excess alcohol), or consumes large amounts of acidic foods or drinks, especially fizzy drinks, will suffer from significant damage to the enamel. This will leave the teeth with a worn appearance, poor in colour, often temperature sensitive with a gradual wearing away of the teeth simply from chewing or grinding teeth against one another. Plaque build-up occurs more quickly on dentine and stained tooth surfaces leading to an increased risk of new tooth decay and gum disease. This is a common finding in ageing adults but should not be considered a normal or acceptable change associated with ageing. These changes can be prevented if they are identified at an early stage. Such detection can only be achieved if adults attend for regular dental examination and dental health assessment. In other words, you don’t have to live with a yellow, dull smile!
Teeth whitening technology
Improvements in the technology used for teeth whitening have increased the degree to which teeth can be whitened. However, remember, while rejuvenation will almost certainly result from this procedure, you cannot guarantee a return to the white teeth of your 20’s. Tooth whitening kits come in various concentrations and generally contain Carbamide Peroxide. The lower concentrations can be obtained over the counter at chemists and in some supermarkets, yet the more effective concentrations can only be obtained through your dentist. Generally, the low concentration kits have only very minimal effect and are more useful in “maintaining” a result already achieved after your dentist has either performed a tooth whitening treatment in the chair or after using a high concentration home kit. The higher concentration whitening kits often contain up to 20% Carbamide Peroxide. There is, unfortunately, a “trade-off” when using these stronger kits in that they may achieve a better colour outcome but they can also lead to anything from mild to very severe tooth sensitivity. This is why they are not available in shops. You need to discuss how susceptible your teeth are to this problem and discuss all the pros and cons of using these more concentrated forms of hydrogen peroxide producing kits. It is therefore strongly recommended that you visit your regular dentist for the best treatment solution for your situation.
Dry mouth when you are 50 years and older
As we age, saliva flow in the mouth can be reduced leading to a dry mouth. This is a condition called Xerostomia. It can be caused by medical conditions affecting the salivary glands directly. It can also result in radiotherapy for cancer in the head and neck region and can result as a side effect of a range of medications, the most common being blood pressure medications and antidepressants or sedatives. It is very important to ensure that as you age you drink sufficient water every day, especially those living in warmer climates. A failure to drink adequate water will result in the body naturally conserving water by reducing the loss of water in a number of other ways. It does this by reducing sweat and minimising the excretion of tears and saliva leading to dry eyes and a dry mouth. It is important to disclose the medications you are taking to your dentist or oral health care professional including over the counter medications as this may allow drug interactions and side effects to be identified. With regard to adequate saliva, patients with very fine bubbly saliva that results in spitting when you are talking can be a sign of poor quality and reduced quantity of saliva. It can indicate a degree of dehydration, a condition that is extremely common in those living in the tropics. If you are experiencing a dry mouth you may also have a sore throat, difficulty speaking or swallowing, and dryness in the nasal passages, which can all be uncomfortable.
Effects of reduced saliva for patients 50 years and older
Reduced saliva is extremely detrimental to your oral health. Saliva is the first line of defence in the mouth against infection and the most important means of preventing dental decay and clearing acid from the mouth and in protecting the teeth. Saliva contains various salivary enzyme systems that assist in the fight against bacterial plaque and helps inhibit the growth of dental plaque. Saliva also flows continuously in response to taste sensation or the presence of food in the mouth and helps to return the acid-alkaline balance of the mouth to a neutral value after consuming foods or beverages containing fermentable carbohydrates (sugars). This is an important mechanism to protect the teeth against the acid attack that can lead to demineralisation of the teeth and the development of dental decay and cavities. Reduced saliva in the elderly increases their susceptibility to the development of decay of root surfaces of teeth with an increased need for fillings. Many elderly people have suffered from some gum recession. This leads to exposure of the root surface dentine to the oral environment without any covering of enamel. This is a very common problem, particularly in those elderly patients who rely on carers to maintain good tooth cleaning. Poor tooth cleaning allows plaque to build up on root surfaces and then acid produced in the plaque from the sugars in the diet attack the root surface leading to demineralisation and cavity formation. Patients with a dry mouth need to see their dentist and dental hygienist to discuss how to manage this problem. There are special mouth wash and tooth paste systems to help maintain a moist mouth and constant sipping of water throughout the day will help to keep the oral tissues comfortable. However, much of the protection provided by natural saliva will be lost and cannot be replaced. These patients suffering from Xerostomia need regular dental preventive dental care and advice.
Oral care for patients 50 years and older
Sadly in many nursing homes and geriatric care facilities oral health care is performed poorly by nursing staff and care staff that have received inadequate training in this oral care role. All members of the health care team who choose to work in geriatric health should receive far more education in this very important area of the overall care of their patients. Regular visits of dental hygienists to the facilities to discuss and educate on subjects concerning oral health would result in a dramatic improvement in the oral care provided for this at-risk population group.
Oral cancer for patients 50 years and older
According to The World Health Organisation and The Oral Cancer Foundation, the chance of being diagnosed with oral cancer increases with age. Increased oral cancer risk has been found to be associated with a history of smoking of any sort, alcohol use particularly involving the consumption of spirits and a genetic history of cancer. However, anyone can suffer from  cancer so it is important to check for it regularly. Unfortunately, only about half the patients who suffer from oral cancer survive five years. Improved survival is seen in those patients who are diagnosed in the early stages of oral cancer. The longer the lesion has been present, the poorer the outcome. During dental examinations, dentists include an examination of all the oral soft tissues in the mouth and this provides the best chance of finding such conditions. Therefore, it is imperative that all elderly patients irrespective of whether they have teeth or not, receive a detailed oral examination at least once a year.
cancer so it is important to check for it regularly. Unfortunately, only about half the patients who suffer from oral cancer survive five years. Improved survival is seen in those patients who are diagnosed in the early stages of oral cancer. The longer the lesion has been present, the poorer the outcome. During dental examinations, dentists include an examination of all the oral soft tissues in the mouth and this provides the best chance of finding such conditions. Therefore, it is imperative that all elderly patients irrespective of whether they have teeth or not, receive a detailed oral examination at least once a year.
Tooth loss for patients 50 years and older
Even though tooth loss is becoming less common due to improved oral health education, better dental care and access to topical and systemic fluoride, tooth loss continues to be a sad reality of life for many patients, particularly in rural areas, in indigenous Australians, Torres Straight Islanders and certain immigrant groups. Tooth loss can be caused by extensive tooth decay and by aggressive forms of gum disease. Tooth loss is still a reality for a large number of people. Despite the knock-on effects of premature tooth loss, it is often the cost of treatment and difficult access to obtain treatment that continues to present a barrier for many people obtaining good quality dental healthcare. While tooth loss can lead to further problems, it is the initial preventive advice, improved diet and better access to dental care for many that remain a problem to be solved in our wider community. However, for those people who can access advice and treatment, losing a tooth can lead to reduced ability to chew, altered speech, deterioration in appearance and movement of the remaining teeth with bone loss on healing.
My messages are:
- Research what a healthy diet includes so you minimise the amount of sugar available to your plaque.
- Avoid sugars, including hidden sugars in processed foods.
- Find out how to remove bacterial plaque from teeth effectively by seeing a dental hygienist.
- Visit a dentist for a dental examination every year to identify any dental disease or oral cancer as early as possible.
- Be sure to visit your dentist promptly if you think you may have a cavity as it will get bigger the longer you leave it.
- Don’t put off seeing a dentist if your gums bleed when you brush your teeth effectively, remember, HEALTHY GUMS DO NOT BLEED.
Treating early dental disease is easy, painless, quick and cheaper than waiting until the only option is to remove teeth. If you are interested in any of the topics covered above, please visit the website, patient information centre and click on Educational Articles where you will find a wide range of subjects covered in several articles written specifically for patients. If you have experienced any of these conditions or would like to find out more about oral health in your as you reach age 50 and beyond, call the team at NQ Surgical Dentistry to organise a consultation.
contact the friendly team at NQ Surgical Dentistry today on (07) 4725 1656 or call in to see us at 183 Kings Rd, Pimlico QLD 4812
BOOK AN APPOINTMENT
CALL US TODAY
07 4725 1656
